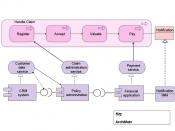
The purpose of adjudication is to resolve disputes so that you don't have to have an expensive and long process in court. It is a process of the examination of claims and determining the outcome of these claim benefits. When the claim is filed and received goes through a 5 stage process to determine how the claim should be paid, (1) initial processing, (2) automated review, (3) manual review, (4) determination, and (5) payment. The purpose of this flow chart is to show you the steps you must take and explain the process of each step and what the purpose is for.
5 STEPS OF THE ADJUDICATION PROCESS
Start
Payers first perform initial processing checks on claims, rejecting those with missing or clearly incorrect information: This will determine if reimbursed each insurer has their own way of claim approval but the process is basically the same.
Claims are processed through the payer's automated medical edits: Once claim is received it has to go through a comprehensive review that is performed by a computer software program that is designed to find errors or discrepancies on the claim form by scanning each claim to make sure information is correct and all necessary information is present on the claim and it conforms to the insurer's policies.
This is called editing and any errors found can cause the healthcare provider not to be reimbursed by the insurer.
A manual review is done if required: This process is done only if the claim fails it can be denied or sent to an insurance examiner for review this is done manually.
The payer makes a determination of whether to pay, deny, or reduce the claim: After the completion of the adjudication process the insurance company sends a letter to the one who filed the claim...