Borderline Personality Disorder affects an estimated five million Americans. Patients with BPD make up 20 percent of psychiatric inpatients and 10 percent of psychiatric outpatients (American Psychiatric Association [APA], 2000). The symptoms of borderline patients are similar to those for which most people seek psychiatric help: depression, mood swings, the use and abuse of drugs and alcohol as a means of trying to feel better; obsessions, phobias, feelings of emptiness and loneliness, inability to tolerate being alone, problems about eating.
There are four important objectives in understanding BPD: The history, the symptoms, the causes, and to explore possible therapy options for individuals with BPD. The term "borderline" goes back a long way. Originally thought to be at the "borderline" of psychosis, people with borderline personality disorder (BPD) suffer from a disorder of emotion regulation.
For centuries, European society excluded people regarded as "insane" from normal life, confining them to asylums or driving them from one town to another.
When the 18th century came around, a few doctors began to study the people in asylums. They discovered that some of these patients had not lost their power to reason: they had a normal grasp of what was real and what was not. Their "crime" was the terrible suffering from emotional anguish through their impulsiveness, rage, and a general difficulty in self-government caused others to suffer. They seemed to live in a borderland-between outright insanity and normal behavior, and feelings.
These people (who were neither insane nor mentally stable) continued to puzzle psychiatrists for the next one hundred years. It was in this "borderland" that society and psychiatry came to place its criminals, alcoholics, suicidal people, emotionally unstable, and behaviorally unpredictable people--to separate them from both those with a defined psychiatric illnesses on one side; and the "normal" people at the other...

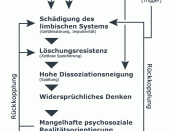
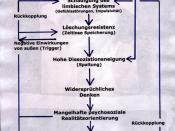
Interesting.
i particularly liked the way the writer of this essay has linked historical perspectives of mental illness to the present day. This essay has got personality, opinion and knowledgable perspective. thankyouxxx
beelyboppers
1 out of 1 people found this comment useful.