Decreasing Brain Matter in Schizophrenia
Abstract
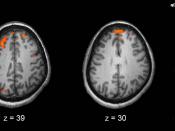
Schizophrenia is a primary focus in the medical community due to its complexity, the lack of understanding about it, and increasing need for treatment in the field of neuropsychiatry. It is thought that the progression of the disorder influences its severity of schizophrenia, which in turn is perceived to be caused by degeneration in the hippocampal, cerebral and peripheral gray matter, peripheral white matter and the total brain volume. This information was obtained through comparative mathematical analysis though the use of MRI scans. These regions (gray and white matter, and hippocampal regions) have confirmed that there is a progressive reduction or brain matter volume in schizophrenics, in contrast to comparative healthy test subjects.
Introduction
Schizophrenia, as defined in the DSM-IV (American Psychiatric Association 1994), is classified as a serious psychotic disorder affecting the mental state (what a person thinks and feels) and stability of oneself in society.
This disorder can occur in any age group, but is typically found in people aged 15 to 35. Schizophrenia affects approximately 1% of the population. Common symptoms, which must be present for one consecutive month in order for a diagnosis to be made, include: delusions, prominent hallucinations, catatonic behaviour, disorganized speech, etc.
In previous findings of gray matter depreciation in schizophrenics, it was found that there was a consistent degeneration of total brain matter volume (Baare et al. 2002). This includes the frontal lobe and frontal and superior temporal gray matter regions. However, there are uncertainties as to whether brain depreciation progresses in severity or remains stable over the course of the psychiatric disorder. Also previous studies have been inconclusive in determining whether there is a correlation between schizophrenia patients and changes in hippocampal (the part of the brain that plays a significant role in memory, attention,