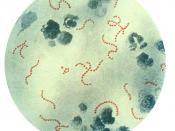
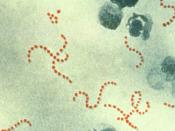
Group A Streptococcus (Flesh-Eating Bacteria) INTRODUCTION Group A Streptococcus can normally be found in the throat and on the skin. This strain of Strep causes mild to severe infections such as strep throat. A more virulent strain of GAS causes necrotizing fasciitis. Invasive infections of GAS are found in areas where the bacteria is not usually present.
Streptococcus pyogenes infects the host by the following sequence of events. 1.The bacteria produces pyrogenic exotoxins A and or B, which can be found in severe infections. The exotoxins are toxins that are released extracellularly as the organism grows.
2.The exotoxins and the surface M-proteins act as superantigens. Superantigens cause the host damage by massive stimulation of the immune system.
3.The antigen binds to the Beta-chain of the T-cell receptor in a location that is not the normal binding site.
4. Leads to overproduction of T-cells in the area of bacterial growth 5.
The T-cells secrete large amounts of effector cells causing inflammation, tissue destruction, and death in approximately 30% of cases. This tissue destruction is what gives this strain of Strep the name "flesh-eating bacteria". The bacteria spread so quickly because they secretes streptokinase, a fibrinolytic substance that dissolves clots that would have otherwise prevented further growth and invasion.
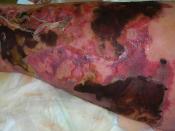
NECROTIZING FASCIITIS Necrotizing fasciitis is an infection of the soft tissue that causes necrosis of fascia and subcutaneous tissue. It most commonly affects areas of the groin, abdomen, or extremities, but can attack almost anywhere. It is one of the fastest spreading infections known, and without treatment can lead to death.
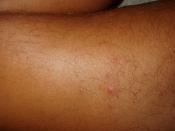
The infection usually develops in the following manner: Opening in skin is present Exposure to Strep Type A bacteria, usually an invasive strain Bacteria grows and releases toxins Discomfort in region where bacteria infected skin Pain worsens and flu-symptoms develop Area swells, becomes red, hot and painful Large, black blisters form as infection spreads and develops The opening in the skin most often associated with flesh eating bacteria is some kind of minor trauma to the skin. Other possibilities include surgery, giving birth, or broken bones. All it can take is a little pinprick and the right conditions. The whole process occurs within a week and a few have died in as few as 24 hours. Therefore, time is of the essence in diagnosing this infection in order to stop it before it progresses too far.
WHO IS AT RISK? Necrotizing fasciitis can develop in any person; however those most at risk are: Children younger than the age of ten Elderly older than the age of 74 Those with underlying chronic illnesses such as cancer or heart disease.
SYMPTOMS Skin painful, red, hot, swollen Skin develops a violet discoloration with blisters Fever Rapid heartbeat Sweating Chills Nausea Dizziness Weakness Shock Vomiting Diarrhea Dehydration Necrotizing fasciitis can lead to death if it is untreated, but when diagnosed and treated this can be prevented. The sooner it is caught, the easier it is to treat. However, because most of its symptoms are flu-like, it can be difficult to diagnose until it is later on in the progress of the infection.
TREATMENT AND PREVENTION When diagnosed early it is possible to stop Necrotizing fasciitis. The treatment necessary depends on how far the infection has progressed. Possibilities include: Powerful antibiotics given intravenously Drainage and removal of infected tissue Amputation of the infected limb There is no sure prevention of Necrotizing fasciitis, however there are ways one can decrease their risk: Clean any skin injuries thoroughly and apply an antibiotic ointment.
After a skin injury watch for symptoms and consult a doctor immediately if symptoms are observed.
Be cautious of spreading any type of strep infection.
REFERENCES Information on Group A Streptococci, from the Centers for Disease Control http://www.cdc.gov/ncidod/dbmd/diseaseinfo/groupastreptococcal_g.htm Necrotizing Fasciitis of the Head and Neck, by Troy A. Callender, MD http://www.bcm.tmc.edu/oto/grand/123192.html