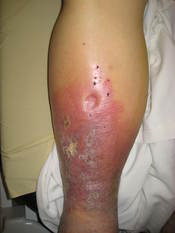
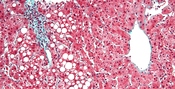
A 46 year old African American woman was admitted 6/24/08 to the ICU at LBJ Hospital with a primary diagnosis of acute pancreatitis. She had come to the ER with diffuse abdominal pain that was increased in the left upper quadrant, ascites, weakness and anorexia. She also was having nausea, vomiting, and diarrhea for two weeks. Her stools were watery with a yellow, mucous appearance. Past medical history includes: Pancreatitis, discoid lupus erythematous, GERD, asthma, and bipolar disorder. Past surgeries include: Two previous cesarean sections, appendectomy, whipple procedure with partial hepatectomy (2006), gastric bypass surgery (1999). Social History: Smokes 6 cigarettes a day, chronic alcohol use, and cocaine. She is currently living with her husband.
A diagnostic paracentesis was performed on 6/25/08 as bacterial peritonitis was suspected. Patient became hypotensive and went into shock. She was admitted to MICU at that time. Respiratory function declined and an endotracheal tube was inserted and client was placed on a ventilator.
An exploratory laparotomy was performed on 6/26/08. The bowel was edematous and a small bowel enterocutaneous fistula was discovered. There was a pancreatic abscess with necrosis in the surrounding tissue. Some cirrhosis of the liver was also noted. Nine enterotomies were repaired and necrotic tissue was debrided. Cultures were positive for vancomycin resistant enterococci strain. Contact precautions are being maintained. The abdominal incision is left open with two drains connected to a wound vac draining serosanguineous fluid. Packed RBCÃÂs, fresh frozen plasma, and platelets were administered. Peritoneal lavage is performed every 48 hours for debridement.
This patient is at nutritional risk due to many factors. First the client has a history of chronic alcohol abuse which is the most common cause of cirrhosis and pancreatitis (Lewis, 2007). The chronic vomiting, diarrhea, and anorexia depleted fluids and electrolytes and nourishment. Also due to...