Post Traumatic Stress Disorder
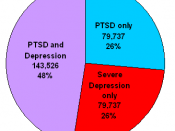
Many of the inmates that we have seen often have one diagnosis that is intertwined with their major problems: Post Traumatic Stress Disorder (PTSD). How do we effectively help these people recognize and deal with the traumatic events in their lives so that they can deal with PTSD and possibly prevent this disorder from manifesting into further psychiatric problems?
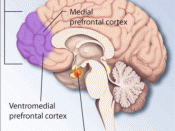
Someone with PTSD may experience unwanted memories when exposed to certain stimuli; sometimes these stimuli are real or perceived. Many times these people turn to substance abuse to deaden troubling symptoms or develop a concurrent psychiatric problems, such as eating disorders, OCD, or multiple personality disorder. A PTSD episode activates the fight or flight response from the sympathetic nervous system. When triggered inappropriately in PTSD, the fight or flight response can have negative social consequences such as chronic anger, violence, aggression, disassociation and an altered self-perception.
These feelings many times lead to illegal behavior and incarceration.
Diagnosis can be difficult because signs and symptoms vary among different people. Careful clinical interviews are used to evaluate the client's psychological status. Most treatment includes a combination of patient education, drug therapy, and psychotherapy. Studies have shown that letting someone just talk about a catastrophic event in their lives reduces the likelihood of developing PTSD. In addition to professional help, there are a number of techniques that help prevent problems from escalating, the clinician should:
Provide a calm, safe environment.
Meet the clients basic needs by addressing fatigue, hunger, loneliness.
Establish trust by assuming a positive, consistent, honest, and nonjudgmental attitude.
Communicate clearly and honestly.
Help your client to realize that his/her symptoms are common reactions to stressors.
Help your client feel that they are not responsible for their disorder.