A young man by the name of RY was hospitalized for severe trauma and injuries to the brain. Upon further examination and observation doctors concluded that RY suffered from Cotard and Capgras Syndrome. Capgras Syndrome is a rare disorder in which a person holds a delusional belief that an acquaintance, usually a spouse or close family member, has been replaced by an identical looking imposter. Cotard Syndrome is also a rare disorder in which the individual suffers from delusion. However in Cotard Syndrome the person may suffer from both hallucinations as well as delusions. Those delusions can range from the individual believing that they have lost organs, blood, body parts, even their sole or life. In more profound cases the individual believes he or she does not exist. Both Cotard and Capgras Syndrome can coexist in patients, although rarely. Usually the patients who suffer from these disorders also have some form of Schizophrenia.
These syndromes can also be apparent in people who have suffered severe trauma or injury to the brain.
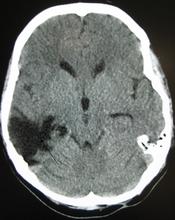
In a Case Study done by the Australian and New Zealand Journal of Psychiatry, RY a 17 year old man was diagnosed with Cotard and Capgras Syndrome. RY was admitted to the hospital after suffering a severe and traumatic brain injury. The injury to RY's brain was so severe that it left him non responsive, and completely dependent on others for basic care and needs. After completing a CT scan, it was concluded that RY had hematomas in the right thalamus and the left Basal Ganglia among other injuries.
Because RY's Basal Ganglia, the area of the brain in which anxiety, motivation, motor behavior, feelings and movement are controlled, was physically compromised RY could possibly be both physically and mentally forever changed. Some of the problems associated with a compromised Basal Ganglia are, anxiety nervousness, panic attacks, physical sensations of anxiety, tendency to predict the worse, and sometimes conflict avoidance. All of the associated problems of such an injury could eventually lead the injured individual to exhibit odd random behavior.
During a 16 week recovery of auditory, occupational, and physical therapy with active participation in daily activities RY was able to provide minimal self-care for himself. RY was soon able to vocalize on a single word level. Although RY was able to achieve those levels of optimal performance he began to display abnormalities in his cognitive development. RY started to develop the belief that vision was impaired. After further testing doctors refuted any possibility that RY's vision was in some way impaired or damaged. During RY's recovery it was indicated by hospital staff that RY had apparent delusional ideation, "super imposed on Post Traumatic Amnesia" Butler, (2000). In the morning RY would appear perplexed, fearful, and have feelings of death dismemberment, persecution, or torture. RY was often hostile and on several occasions accused the hospital staff of murdering his family members. RY, when visited by his father, would become agitated and restless. RY would examine his fathers face before accusing him of being a "criminal double who had taken his fathers place" Butler, (2000).
It was stated that RY would often refer to his-self as "dead and detained in Hell against his wishes" Butler, (2000), but at other times later in the day, he was "mildly euphoric" with no obvious elements of "dysphoria or fearful apprehension" Butler, (2000). Because of the inconsistencies in RY's behavior, hospital staff noted the behavior as, "a simple delirium and depressive disorder, with, psychotic or melancholic features" Butler, (2000). It was later concluded that RY's delusion and "depersonalization" were maintained by the vivid dreams and nightmares he was unable to differentiate from ordinary reality. RY was prescribed Olanzapine (antipsychotic medication) to treat the ideation which ultimately worked, however RY still even after treatment remained agitated and somewhat mistrustful of his father. After further treatment with Olanzapine, RY was eventually discharged to a regional brain injury unit for further rehabilitation. RY was gradually taken off the medication and there was no presence of any delusions or ideations.
The Case Study done on RY concluded that he in fact did suffer from hallucinations, delusions, and at times intense emotions toward others all of which are associated to Capgras and Cotard Syndrome. The hallucinations and delusional thoughts and behavior RY exhibited could arguably be considered symptoms of Schizophrenia. Schizophrenia is a disorder in which the sufferer's personality disintegrates and their thoughts and perceptions are distorted, and emotions are blunted. RY as reported by hospital staff would often have hallucinations after awakening from sleep, but throughoutthe course of the day the delusions and hallucinations would subside. Later in the day RY would become more sociable and cognitively oriented. The delusion RY suffered from was the belief that he was "dead or detained in Hell against his wishes". These hallucinations were that of an "Acute Phase" Gerrig, Zimbardo, et al. (2008). During Acute Phases of Schizophrenia the positive symptoms (hallucinations and incoherence) are prominent. However, throughout the course of the day RY's mood was described as "mildly euphoric" Butler, (2000). The mood swings RY had during the day could, in some aspect, reinforce the idea that he did possibly suffer from both Capgras and Cotard Syndrome with maybe an underlying undiagnosed case of Schizophrenia.
Because the symptoms associated with Schizophrenia are so vast, subtypes have been outlined to provide a better understanding and explanation of Schizophrenia. Because RY suffered from hallucinations and delusions he could fit into the subtype of an Undifferentiated Schizophrenic Gerrig, Zimbardo, et al. (2008). An Undifferentiated Schizophrenic is an individual who has prominent delusions, hallucinations, incoherent speech or grossly disorganized behavior that fits more than one type. After medication in accordance with rehabilitation therapy RY was eventually taken off the Olanzapine with no apparent false ideations or delusions. RY's Schizophrenia could have then been considered a "past episode" marked with positive symptoms (delusions, hallucinations, and intense emotions) that eventually subsided Gerrig, Zimbardo, et al. (2008). This occurrence was that of a "Residual Schizophrenic" Gerrig, Zimbardo, et al. (2008).
Residual Schizophrenia is the process in which the disease is entering remission or becoming dormant. RY was able to eventually be discharged from the Rehabilitation facility free of any previously diagnosed conditions. The treatment of his hallucinations, and delusions were effectively treated with the Olanzapine. Doctors concluded that RY no longer exhibited any symptoms of Schizophrenia, Cotard or Capgras Syndrome.
The Cotard and Capgras Syndrome RY suffered with are both delusional disorders that are often most commonly associated with individuals who also suffer from Schizophrenia. Because RY's behavior was so random his Schizophrenic behavior could be that of some who could have been diagnosed with Undifferentiated Schizophrenia. Despite the persistent hallucinations and delusions doctors were able to effectively treat and eliminate RY's ideations and false feelings sending his disorder into remission. The mere fact that RY's symptoms were in remission could lead one to believe RY was also a Residual Schizophrenic. After release from the Brain Injury rehabilitation facility RY was no longer on any medications nor did he have an ideations, hallucinations or delusions.
Reference ListButler, P. V. (2000). Diurnal variation in Cotard's syndrome (copresent with Capgrasdelusion) following traumatic brain injury. Australian and New Zealand Journal of Psychiatry, 34, 684-687.
Gerrig, R. J., & Zimbardo, P. G., et al. (2008). Psychology and Life (18th ed.). Boston,MA: Allyn & Bacon




![Laying cornor [i.e., corner] stone, Columbia. Pres. Butler & Dean Wheeler (LOC)](https://s.writework.com/uploads/13/133219/laying-cornor-e-corner-stone-columbia-pres-butler-dean-wheel-thumb.jpg)