January 31, 2006There are a lot of diseases today, some diseases we know a lot about and are curable others are not; then there are the diseases we just donÃÂt know a lot about and have no cure. Scleroderma is a disease that we know a little bit about but have to cure. Patient and their families that do encounter the disease have questions. Questions like what is Scleroderma, we know there is no cure but is there treatment for it, and what is the prognosis?The word scleroderma comes from two Greek words: ÃÂscleroÃÂ meaning hard, and ÃÂdermaÃÂ meaning skin. Scleroderma is an autoimmune disease of the connective tissue. It is a chronic disease. ÃÂScleroderma is characterized by the formation of scar tissue (fibrosis) in the skin and organs of the body.ÃÂ(Medifocus, 2006) This leads to thickness and firmness of involved areas. Scleroderma is also referred to as systemic sclerosis.
The cause of Scleroderma is unknown. Fortunately, scleroderma is relatively rare affecting approximately 300,000 persons in the United States. The disorder most commonly occurs in women between the ages of twenty and forty; however men and children can be affected as well. The disease is not contagious and is not thought to be inherited.
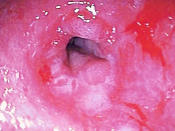
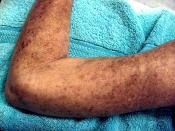
There are two categories of Scleroderma diffuse and limited. The diffuse form of scleroderma is involves symmetric thickening of skin of the extremities, face, trunk (chest, back, and abdomen) which can rapidly progress to hardening after an early inflammatory phase. Organ disease can occur early on and be serious. Organs affected include the esophagus, bowels, lungs (with scarring), heart, and kidneys.
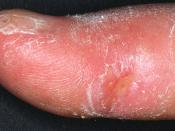
The limited form of scleroderma tends to be toward the skin of the fingers and face. The skin changes and other features of disease tend to occur more slowly than in the diffuse form.
ÃÂThe diagnosis of the scleroderma syndrome is based on the finding of the clinical features of the illnesses. Nearly all patients with scleroderma have blood tests which suggest autoimmunity, antinuclear antibodies (ANAs). A particular antibody, the anticentromere antibody, is found almost exclusively in the limited form of scleroderma. Anti-Scl 70 antibody (antitopoisomerase I antibody) is most often seen in patients with the diffuse form of scleroderma.ÃÂ (Medicine Net. Inc., 2006) Other tests are used to evaluate the presence of any internal disease. These may include upper and lower gastrointestinal tests to evaluate the bowels, chest x-rays, and lung function tests to examine the lungs, EKG and echocardiograms to evaluate the heart and lung arteries.
Currently there is no cure for Scleroderma. Even though there are no cures for the disease (or syndrome) there are treatment options. The treatment options depend on the location, or if it is diffused or limited. In general, medications that may be used include immunosuppressive agents, antifibrotic agents, anti-inflammatory agents, vasodilators, and angiotensin-converting enzyme inhibitors (Medifocus, 2006). In rare cases, when symptoms of systemic sclerosis become severe, surgery may be recommended.
The prognosis varies for patients depending on which type of scleroderma they have. Scientist says that it is often difficult to make a prognosis in the early stages of the disease. Scientist also say that the prognosis for patients with limited sclerosis who do not develop pulmonary hypertension is good; but men who develop the disease, patients with diffuse scleroderma, and patients who experience kidney, lung, and heart involvement generally have a worse prognosis.
ReferencesMedifocus, (2006). Scleroderma. Retrieved January 7, 2007, from Scleroderma guide book Website: http://www.scleroderma-info.com/guide_detail.aspMedicine Net, (2006). Scleroderma, symptom and treatments. Retrieved January 7, 2007, fromScleroderma cancer Web site: http://www.medicinenet.com/scleroderma/index.htmKleinert, S., Tony, H.P., & Kneitz, C. (Oct 2006)Systemic sclerosis./SystemischeSklerose. In Der Internist, 47, p1051(12). Retrieved January 8, 2007, from HealthReference Center Academic via Thomson Gale: http://find.galegroup.com/itx/infomark.do?&contentSet=IACDocuments&type=retrieve&tabID



Rip off ?
Its all on the net for any one to google, what's the value addition in this essay?
Please make an effort to include any practical experiences in diagnosis or treatment.
0 out of 0 people found this comment useful.