In today's society, it is commonly assumed that people are able to receive the medical treatment that they require. The people that aren't able to receive the specialists or procedures needed are typically instances that society doesn't hear about or rather chooses to overlook because the people in this predicament are representative of the lower echelon of the population, the people we would rather not associate with or even claim as fellow members of our race. This is extremely unfortunate, and I believe that when someone requires a certain specialist for a condition they suffer from it is of utmost important that they have access to the medical care they need.
Now suppose you are a physician and you meet a patient who has not been treated for a severe chronic condition for almost a decade. This patient cannot afford to see the specialist that he desperately requires; indeed he is only coming to you because you see patients on a sliding scale; yet you are not trained properly to treat him for his conditions.
He has many heart problems, yet you only have your license as a family practitioner. What do you do? Is it okay for you to treat this patient even though the level of care he requires lies beyond your threshold of expertise, or should you treat him to the best of your capability, assuming that no one else will? On top of everything else, what if this patient is not consistently compliant, and thus poses a huge liability, both to tour practice and his own health?During my internship at North Shore Health Center, I became very familiar with the case of one of Dr. Girn's most controversial patients. This patient came to visit him one day, complaining simply of a rash on his hand, but with the intent to also establish a primary physician. As Dr. Girn was gathering and looking over his medical history, however, he began to realize that there was much more to the picture than meets the eye. Some of the symptoms that the patient reported in his preliminary paperwork include swelling or edema in the feet, ankles, and hands, shortness of breath at night, and redness, swelling, pain, weakness, or numbness located in the feet and legs. He also claimed asthma and heart disease as existing medical conditions.
In the patient's family history, he listed that his father suffered from a history of heart disease and strokes, while his mother died from heart disease at the age of 63. The patient also wrote that he was hospitalized at Porter Memorial in 2001 for a heart attack. After obtaining his medical records from other facilities, Dr. Girn came to find out that the patient had also had three stent placement surgeries.
When Dr. Girn met with the patient, he discovered some more information pertinent to our case. The first appointment with Dr. Girn was in September of 2008. He had not seen a cardiologist or had any sort of lab work done since his hospitalization in 2001. Also, he had stopped taking his medications shortly after he was released seven years prior. This is very frightening news with someone with such a strong history of heart disease in their family.
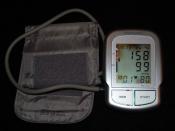
To give you an idea of the shape this patient was in when he first came to visit Dr. Girn, I will share some of his vitals with you. His pulse was 132, compared to the average of 75, he is five feet and nine inches tall, he weighs 402 pounds, he is 44 years old, and his blood pressure is an incredible 184 over 112. From these statistics Dr. Girn came to the conclusion that the patient has extreme hypertension, and obviously needs to resume his high blood pressure medicine as soon as possible or else poses a huge health risk to himself. Dr. Girn also discovered that the patient suffers from tachycardia, and therefore his heart has to work very hard to circulate blood to his body in order to be working at the rate it is. He is extremely obese, which simply increases all these risk factors exponentially, as well as his habits of smoking and drinking. After obtaining all this information and taking into account the fact that the patient hadn't taken medicine for seven years, Dr. Girn asked himself, how do I even begin to treat this patient? More than that, what were the underlying causes to his health problems he was experiencing?In order to best help the patient, Dr. Girn had to completely understand his medical conditions, which required him to leave his comfort zone and travel out of his area of expertise. He researched the symptoms and he came up with three major diagnoses for the patient, congestive heart failure, hypertension, and coronary artery disease.
After learning what the patient was diagnosed with, I had several questions before I could delve any further into the ethical dilemma. These questions included signs and symptoms of these diseases, causes of these diseases, progressions of these diseases, and treatments for these diseases. I managed to scrounge up most of this information on the internet; however Dr. Girn was a tremendous resource as well. I also asked Dr. Girn to look into the patient's family life to find out more information for me as to how he was being supported, and why he didn't have insurance.
Returning to the patient diagnoses, hypertension, or HTN, is a medical condition marked by the chronic state of elevated blood pressure. There are different stages of high blood pressure, and different levels that you should get treatment regarding what diseases you suffer from, but according to the UK guidelines, if you suffer from heart disease as our patient does, you should seek treatment when your blood pressure is greater than 140/90.
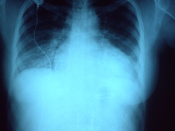
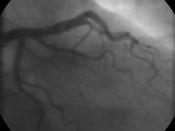
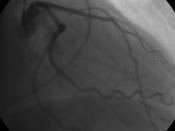
Coronary artery disease, also known as CAD, is a condition in which plaque, made of fat, cholesterol, and calcium, builds up inside the coronary arteries that supply your heart with oxygenated blood. This buildup is known as atherosclerosis, and causes blocked blood flow, as well as an increased risk of a clot. CAD is the leading type of heart disease, and can lead to other conditions if not treated with medicines, procedures, or lifestyle changes. Our patient suffers from this due to his history with stent placements.
Congestive heart failure, or CHF, is a condition in which the heart's function as a pump to deliver oxygen rich blood to the body is inadequate to meet the body's needs. This can be caused by a variety of things; coronary artery disease, hypertension, (both of which our patient has) alcohol abuse, and disorders of the heart valves, as well as others. There is a blood test that can be used to determine whether a patient has CHF called a brain natriuretic peptide level which elevates with heart failure, which indicated our patient has this. Some symptoms that also indicate the presence of CHF include: swelling of the lower extremities, shortness of breath due to fluid in the lungs, an increase in urination, particularly at night, as well as nausea and abdominal pain.
It is vital to note that treatments for these conditions are not cheap, and they are not simple or easy for the uncommitted patient to maintain. The patient must be dedicated to changing his lifestyle, without the doctor having to be act as the driving force. Behavior modifications include a diet low in sodium, helping to decrease his swelling, as well as a low calorie diet, decreasing the patient's BMI and easing strain on his heart. The patient also needs to have different labs and blood work routinely drawn to check for cholesterol levels, WBC and RBC levels, anemia, thyroid function, diabetes, and tests examining kidney function, because abnormalities in these levels can be linked to heart disease. In addition to lab tests, an added expense the patient has to add to his agenda includes various exams done for his heart, such as echocardiograms, stress tests, and possible surgeries. Furthermore, the patient needs to stop smoking and drinking and keep regular doctor appointments, and most importantly, take all medication regularly, which could easily cost hundreds of dollars per month.
Now that I have provided you with the pertinent medical information regarding this patient's case, let me explain a little regarding his personal life. During the years 2001-2008, when the patient did not seek treatment, he lived with he father in a run-down trailer. He did not work because of his extreme lack of motivation and poor health, and was supported by his father. The patient took no initiative to obtain insurance or any sort of employment that I know of until he applied for HIP insurance in October, 2008. This was almost a year after his first appointment with Dr. Girn, which allowed him to continue his treatment, and allowed him to receive the extent of treatment medically necessary.
To recap the information provided with the four-box approach, the patient is suffering from heart disease, caused by CAD, CHF, and HTN. With proper medication, treatments, and behavior modifications, the patient can have a significantly improved quality of life, in comparison to suffering from prior symptoms such as shortness of breath, fatigue, and severe swelling. The patient at first did not want to seem to take care of himself, and only came to Dr. Girn on the premise of his rash, yet through his continued visits I believe he shows a continued dedication to improving his health and seeking treatment. Some other features regarding the patient's personal life include the facts that he didn't have a job or insurance for a significant period of time, and he lived with and was supported by his father.
This patient did not receive the specialized treatment that he needed. Though the patient only visited Dr. Girn on the premise of a rash, Dr. Girn, a family practitioner, continued to see and treat him for his heart disease despite his lack of specialized training, and the patient was unable to pay for the specialized treatment that he needed. A precedent case that we can compare to this scenario is the case of Larry McAfee. Larry McAfee also didn't receive the specialized treatment he needed because of his inability to pay.
Larry McAfee was in a motorcycle accident and became a C-2 quadriplegic, needing a ventilator to survive. After his health insurance ran out, he became eligible for Medicaid. With Medicaid came a constant battle for adequate treatment, because the reimbursement from Medicaid was so low. He was dumped from state to state, even spending several months in the ICU of Grady Memorial Hospital at Georgia. After this, he was placed in Briarcliff Nursing Home, left to stare at the white ceiling with no accommodations whatsoever for his special needs. The patient and Larry McAfee both were neglected and treated with injustice due to their economic situations.
This case does not involve any issues of autonomy or competency, but rather centers around beneficence and nonmaleficence. Beneficence means to help others, while nonmaleficence literally means to not harm others, and implies that physicians technically incompetent to do something shouldn't do it. The ethical dilemma in this case contests the two principles of beneficence and nonmaleficence. One possible resolution, based on the principle of beneficence, involves the patient receiving the best care and treatment that Dr. Girn can provide, even for the patient's heart disease which lies outside of Dr. Girn's specialty. On the other hand, maybe it would be better for the patient to receive no treatment at all from Dr. Girn for his heart disease in order to not risk worsening his condition to a further extent. This would be in accord with the principle of nonmaleficence. While Dr. Girn may be able to help the patient with his treatment and improve his quality of life, it is also possible that through his unspecialized treatment the patient's quality of life may suffer. Which is more important, the patient receiving care, or the patient receiving individualized care for his specific needs?After considering this question, there is another ethical principle that comes into consideration. This principle is justice. Justice is when people are treated impartially, without bias on account of gender, race, sexuality, or wealth. It is easy to see how justice is important in the case with this patient, as he cannot afford his treatment. This means that the specialists that he needs won't see him without advance payment, as is the case with the tests that he requires.
The theory of Libertarianism can be used to support the principle of nonmaleficence. This theory opposes government programs and forced taxation, and view such as equivalent to forced labor. Physicians who believe in libertarianism would rather the government not have a hand in their business and instead be compensated only in cash. This is quite ironic considering the fact that the Medicare and Medicaid system is what has served to help keep our health care system running, ensuring patients receive the treatment they need, and that physicians continue to get paid.
A person arguing from this ethical standpoint would say that the patient has not worked for the treatment he requires; therefore he should not be able to receive it. This may seem extremely harsh, but libertarianism possesses a certain logic. Our current system has definite flaws, in that smarter people with more resources take advantage of the government, while the people who really need the financial support are often left without any assistance whatsoever. Libertarianism would certainly counteract this mindset that many Americans possess, relying on America's piggybank for their clothes and food, rather than their own toil and sweat. Libertarianism, however, also poses many flaws. Many people, without social security or disability from the government, would be required to forgo necessary medical treatment in their elder years due to lack of money. As you can see, libertarianism is not without it's checks and balances.
Virtue Ethics are an ancient philosophy emphasizing knowledge, skill, and empathy. This viewpoint is very interesting, as it can easily support both stands. Dr. Girn technically did not have the knowledge or skill required to treat the patient for heart problems that in fact required a cardiologist, and yet he did because he had such a strong sense of empathy. It could also be argued that just because the American Medical Association requires that you be trained and pass boards in a certain field before you are allowed to practice in that area does not mean that you do not possess the skill or knowledge necessary to treat someone. Out of both of these arguments, I feel that the latter, in favor of beneficence, is the strongest.
Kantian ethics also validates beneficence, the stand that I take. Kantianism tells us that an act is right if it can be applied to and acted on by everyone for good. Kantianism is also very duty-driven; that is, why an act is done is more important than its results. This theory states that there is only one correct motive to act from, and that is to do one's duty, stemming from the desire to be a good person and to do what is right. In this there is also a concept known as 'the veil of ignorance.' This idea affirms that each person is of infinite moral value and worth, and the only way to make any sort of ethical decision is under a veil of ignorance in regards to a person's personal information, such as age, sex, race, health, income, or any other contextual features. Kantianism corroborates with beneficence in that every physician has a duty to their patients, and this duty consists of improving their physical and mental well-being to the best of their capability, regardless of who they are or what place they may hold in society.
In this case Kantianism is clearly practiced. In fact, North Shore's Health Center's founding policy is very similar to operating under the Kantian veil of ignorance, and giving each patient outstanding and indistinguishable treatment, yet providing them with a sliding scale so they can obtain the medical treatments they need. Dr. Girn felt that it was his duty to treat the patient to the best of his ability, and according to Kantianism, the fact that Dr. Girn fulfilled his duty is all that matters.
Another outlook that endorses the principle of beneficence is Utilitarianism. This theory, contrary to Kantianism, states that rather than the motives of the actions, consequences are what count in the end. This also asserts that right acts produce the greatest amount of good for the greatest amount of people. Depending on the circumstances, it may have not been for the greatest good for Dr. Girn to have treated the patient, but in this case it was. Because of the doctor's treatment, the patient received the medication he needed, his blood pressure and cholesterol were lowered significantly, and his symptoms were reduced. Thanks to Dr. Girn's actions, a good deed was accomplished; the patient was given treatment that he could not receive elsewhere to improve his health.
An ethical test that we can put the two opposing viewpoints through is call the Golden Rule. This tells us to treat other people how you would like to be treated in their situation. Considering the ethical dilemma and putting myself in the place of the patient, I would want to be treated with beneficence, having the primary concern being for my health, rather than being to not do me harm. Dr. Girn was an excellent doctor to learn these lessons from, as he was both a very intelligent man, and a very compassionate, grounded, and people-oriented person.
Through this study, my eyes were opened to a new kind of health care. This health care is one that goes above and beyond to help their patients, and does whatever they can so that the patients will be able to afford treatment. This experience let me empathize with both the physician and the patient, and I came out with a better understanding of what really matters that will follow me into my career and through the rest of my life. Now, and throughout my life, I will remember the lesson I learned from this class; no day is worth living if in it you do not go above and beyond to do something good for others.
Works CitedPence, Gregory. Classic Cases in Medical Ethics: Accounts of the Cases and Issues that Define Medical Ethics. 2008. McGraw-Hill: New York, NY.