WHAT DOESN'T KILL THEM ONLY MAKES THEM STRONGER . . .
When penicillin became widely available during World War II, it as a medical miracle, quickly eliminating the biggest wartime killer--infected wounds. Discovered initially by a French medical student, Ernest Duchesne, in 1896, and then rediscovered by Scottish physician Alexander Fleming in 1928, the product of the soil mold Penicillium crippled many types of disease-causing bacteria. But only four years after drug companies began mass-producing penicillin in 1943, microbes began appearing that could resist it because of biological mixing, human amplification and environmental changes. "Antibiotic usage has stimulated evolutionary changes unparalleled in recorded biological history." (Levy) Tuberculosis, gonorrhea, malaria and childhood ear infections are just a few of the diseases that have become more difficult to treat due to the emergence of drug-resistant pathogens. Once resistance develops, all offspring of that bacterium get it. Once the resistant strain is made, everybody who is infected with it will have that resistance problem.
Biological mixing of antibiotics is part of the blame in the fight against diseases. Mutations on antibiotics come into play when drug manufacturers modify an existing antibiotic to overcome resistant bugs. In that case, Bacteria already possess a gene to defeat the antibiotic, and it mutates again to regain mastery over the modified antibiotic. "It is almost as if bacteria anticipate the confrontation of other drugs when they resist one." (Levy)
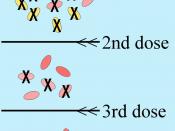
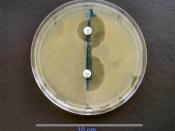
Bacteria acquire genes for resistance in three ways. In spontaneous mutation, bacterial DNA may change spontaneously, as indicated by the starburst (Drug-resistant tuberculosis arises this way). In a form of microbial sex called transformation, one bacterium may take up DNA from another (Penicillin-resistant gonorrhea results from transformation). Most frightening, however, is resistance acquired from a small circle of DNA called a plasmid. Plasmids can flit between bacteria...

Good job
this essay was very interesting and well researched.
keep up the good job
0 out of 0 people found this comment useful.