Treatment of Attention Deficit Hyperactivity Disorder
Medication vs. Alternative Therapies
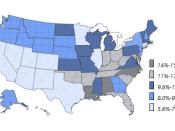
Attention Deficit Hyperactivity Disorder (ADHD) is a chronic, not episodic, illness occurring in 3-5% of the school- aged population. ADHD is characterized by inattentiveness, hyperactivity, and impulsiveness. Most medical professionals classify ADHD as a neurodevelopmental or neurobehavioral disorder that emerges in childhood and may persist into adulthood (McCleery, 2001).
As of today scientists have been unable to pin point a cause for ADHD. Genetic case studies suggest a strong genetic component, though there are other components as well, such as in-utero exposure to cocaine, alcohol, cigarettes, and/or other drugs, or early childhood exposure to lead or heavy metals.
Children with ADHD exhibit hyperactivity, inattentiveness, and impulsivity. ADHD children often have stressed relationships due to the inability to remain on task; they are less compliant with parental instructions, and display more "negative" behavior than children of the same age without ADHD.
These relationship stresses and environmental influences in early childhood can lead to a series of other disorders commonly found in people with ADHD.
ADHD is often paired with a variety of coexisting conditions. Some of the conditions are Oppositional Defiant Disorder (ODD), Conduct Disorder, depression, anxiety, and learning difficulties. These coexisting conditions can result from lack of treatment for the ADHD child. If ADHD is treated as early as it is detected many of these disorders can be prevented from affecting the child now or in years to come (Jensen, 2001).
Treatment for ADHD can be found through a variety of different avenues. In the past, ADHD has most commonly been treated by medicating the child. While this is effective to a certain extent, researchers have found the combination of medication and behavioral treatment to be the most effective in reducing the symptoms, direct and indirect, of ADHD (Wells et...